About PCCRG
Critical care research is challenging
Most treatments patients receive in the emergency department and intensive care unit today have never been evaluated in a clinical trial. Doctors and nurses need to know which of the available treatments produce the best outcomes for patients to provide the best care for critically ill patients. Clinical trials are the best source of information to determine treatments best for patients.
Our Network
Our network has completed more than 20 randomized trials enrolling more than 50,000 patients. Results of these trials, including 8 published in the New England Journal of Medicine or JAMA, identified common, inexpensive treatments that improve patient outcomes (e.g., use of balanced crystalloids rather than saline, video laryngoscopy and bag-mask ventilation during emergency tracheal intubation).
Denver Health Medical Center Ochsner Medical Center University of Washington Medical Center Duke University Medical Center University of Alabama at Birmingham Baylor Scott & White Health UCHealth University of Colorado Hospital Vanderbilt University Medical Center Hennepin Medical Center Wake Forest Baptist Health Brooke Army Medical Center Lahey Medical Center Oregon Health Sciences University Medical Center University of Iowa Medical Center Ohio State Wexner Medical Center Beth Israel Deaconess Medical Center Montefiore Medical Center Our Lady of the Lake Medical Center LCMC Health University of Wisconsin
History
The Pragmatic Critical Care Research Group (PCCRG) was founded in 2013 by Matthew Semler, MD, MSCI; David Janz, MD, MSc; and Todd Rice, MD, MSc of Vanderbilt University to improve care for critically ill patients by using clinical trials to compare commonly used treatments. Over time, the group has grown into a multi-center clinical trials network that includes more than 100 emergency medicine, anesthesia, and critical care medicine physicians, advanced practice providers, nurses, respiratory therapists, and other personnel from 20 health systems across the United States.
Today, the network conducts federally-funded clinical trials in emergency and critical care medicine led by the Coordinating Center (Director: Jonathan Casey, MD, MSCI), Executive Committee (Members: Todd Rice, MD, MSc; Wesley Self, MD, MPH; David Janz, MD, MSc; Adit Ginde, MD; Stacy Trent, MD, MSPH; Matthew Prekker, MD, MPH; Brian Driver, MD; Kevin Gibbs, MD; Derek Russell, MD; and Sheetal Gandotra, MD), and Steering Committee (Chair: Matthew Semler, MD, MSCI) with clinicians and researchers from each hospital. The network focuses on comparing commonly used treatments for respiratory failure, shock, and other common acute illnesses.
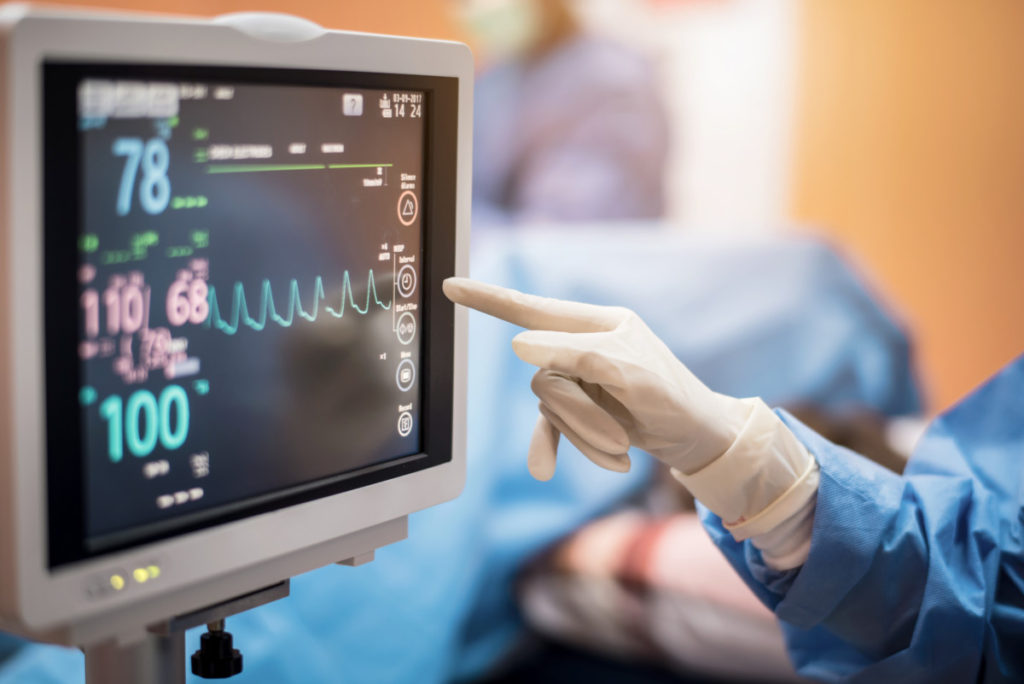
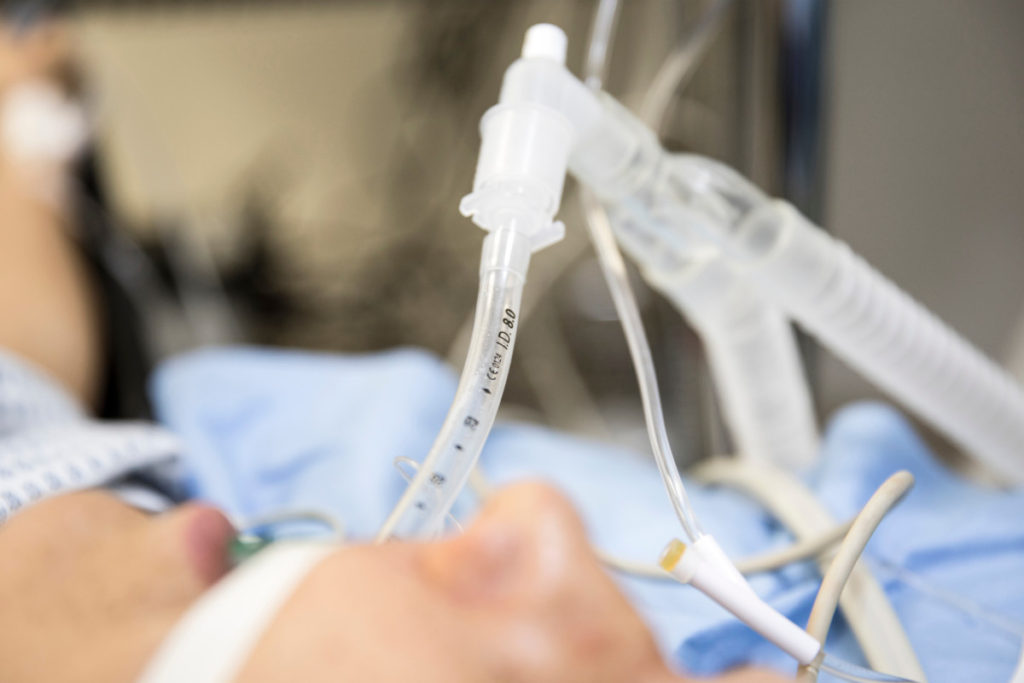
Our Aim
PCCRG aims to continue to use clinical trials to inform the best care for acutely ill patients in real-world settings, to engage patients and community members in acute care research, and to advance methods for implementing clinical trial results to improve care for individual patients through personalized medicine.